Melanoma treatments improving, but prevention and early diagnosis are critical
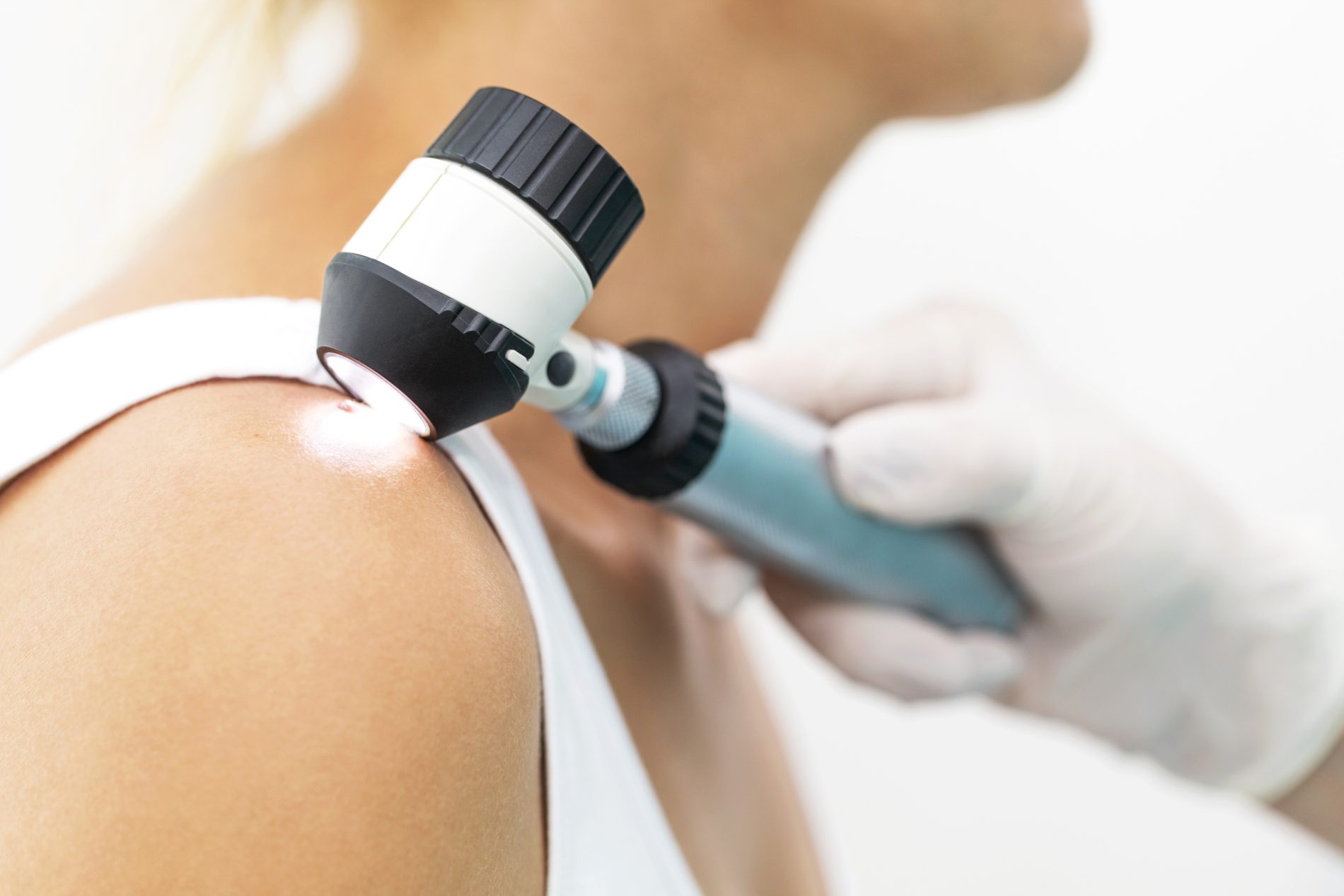
Melanoma is the most dangerous form of skin cancer, and the number of Americans living with the disease continues to rise. Fortunately, melanoma survival rates at all stages have increased greatly due to treatment advances, but prevention and early diagnosis still offer the best chance for survival.
The information below may help you better understand how melanoma presents and how it’s treated.
Causes and symptoms
Melanoma is a cancer of the melanocytes, the cells responsible for pigment in the skin. It’s less common than other types of skin cancer, but the risk for melanoma is increasing as the population lives longer. Common symptoms include changes in the number or shape of moles and the appearance of other unusual spots on the skin.
Melanoma is caused by a combination of environmental and genetic (inherited) factors. Exposure to ultraviolet (UV) radiation from the sun is the greatest environmental risk factor, and that risk is higher for those who have brief but intense sun exposure, as opposed to moderate, long-term exposure. Tanning beds also emit UV radiation.
Fast facts
- Skin cancer is the most common cancer in the United States, and melanoma is the deadliest form.
- An estimated 100,000 Americans will be diagnosed with melanoma in 2024.
- The number of cases among people under age 30 is growing faster than with any other demographic group, soaring by 50% in women since 1980.
- Melanoma affects people of every age, race, and gender. Skin cancer in people of color often isn’t diagnosed until the later stages, making it more difficult to treat.
- Melanoma is not limited to skin cancer, as it can develop anywhere on the body, including the eyes, scalp, nails, feet, and mouth.
SOURCES: Melanoma Research Foundation, American Cancer Society
Diagnosis
If a dermatologist or other doctor identifies a potential melanoma on the skin, the patient usually will undergo a biopsy of the area to collect a tissue sample. The biopsy results are evaluated alongside a detailed review of the patient’s medical history and a comprehensive physical exam. Those diagnosed with melanoma may be treated by a dermatologist, surgical oncologist, or medical oncologist, depending on what stage the cancer is in when diagnosed.
According to 2023 statistics from the CA cancer journal:
- Between 2015 and 2019, 78% of diagnosed melanoma cases were localized (stages 1 and 2), which means the cancer has not spread beyond a small section of skin.
- The five-year survival rate for localized cases from 2012 to 2018 was nearly 100%.
- Only 5% of cases were diagnosed as stage 4, the most dangerous stage. This means the cancer has spread, or metastasized, to other regions and organs of the body.
- The five-year survival rate for those with stage 4 melanoma was 32%, so it’s much harder to successfully treat, but the medical community continues to make strides in improving these outcomes.
Improved treatments
“Melanoma is a deadly cancer, but in the wake of recent advances in medications and treatments for patients, the overall survival rate has improved dramatically over the last decade,” says Kristy Broman, M.D., a surgical oncologist and melanoma researcher at the UAB O’Neal Comprehensive Cancer Center.
Dr. Broman summarizes the range of treatments available at UAB by stage:
Stages 1-2: surgical removal/lymph node biopsy
The simplest and most effective option for local melanoma is to remove the tissue and make sure that any other cancer cells on the edges of the cancerous area also are removed. In many cases, a biopsy of the patient’s lymph nodes will be performed, to determine if the cancer has spread.
Stage 3: immunotherapy and oral medications
Immunotherapy treatments are a newer option for stopping cancer as it spreads by training the body’s cells to find and destroy cancer cells. Immunotherapy is often combined with surgical removal of the cancerous area(s). Oral medications may also be used for certain types of melanoma.
Stage 4: systemic immunotherapy
A combination of the treatments above and systemic immunotherapy (aimed at the whole body) can still be effective in treating stage 4 melanoma.
Treatment at UAB
UAB Medicine is on the forefront of clinical research trials for melanoma. Tumor-infiltrating lymphocyte (TIL) therapy is a promising form of immunotherapy that uses patients’ own altered immune cells to search for and destroy unique cancer cells in their bodies. It’s been available through clinical trials at UAB Medicine but soon will be available to all patients.
Another area of our ongoing research focuses on the timing of immunotherapy with surgery. Performing surgery in between doses of systemic immunotherapy may offer better results than surgically removing the cancer and using immunotherapy afterward.
We all can reduce our risk of melanoma and other skin cancers by limiting direct sun exposure and watching for changes in moles and other unusual spots on the skin. For those who are diagnosed with skin cancer, it can be removed/cured in most cases, and the O’Neal Comprehensive Cancer Center offers treatment pathways for every stage.
Learn more about skin cancer care at the O’Neal Comprehensive Cancer Center.
SOURCES: MedlinePlus.gov, National Cancer Institute




